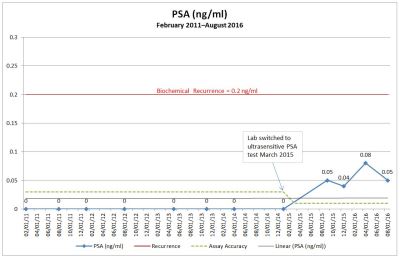
With the change in my PSA over the last year, you can bet that I’ve been seeking every bit of information as to what it means and what to do about it. One of my go-to resources for the latest information in the field has been The “New” Prostate Cancer Info Link.
On 21 September, they published the following blog post that really piqued my interest:
Very early salvage radiation has up to fourfold better outcomes and saves lives
It’s certainly a topic of discussion for my next urologist visit in December. By the study’s definition, I’m still in the “very early” group—the group with the best survival if salvage radiation therapy (SRT) is started while I’m still in that group.
If we have to go down that path, my biggest concern with starting SRT is knowing that we’re actually radiating where the cancer is located. That concern is amplified if imaging can’t show where the cancer’s actually at, and we just radiate the prostatic bed because that’s what makes the most sense. Why risk some long-term, potentially nasty side effects on something so uncertain? (Yes, I know nothing is certain dealing with cancer.)
Of course, this is just one study and making a decision on it alone would probably be unwise.
We’ll just have to wait for the December PSA readings to come back and go from there.
On a happier note, I took a little drive through the country last week to tackle a few things on my travel bucket list: October Odyssey: The Mountain West. Check it out if you want to see what it was all about.