We last left our hero with the beginning of a head cold after his scan and oncologist meeting. And, boy, what a head cold that turned out to be.
Normally, a typical head cold lasts a week or so and you’re back to normal. Not this time. This was the most stubborn virus, hanging on for three weeks and change. It was ugly. So ugly, in fact, that I went to the doctor for help.
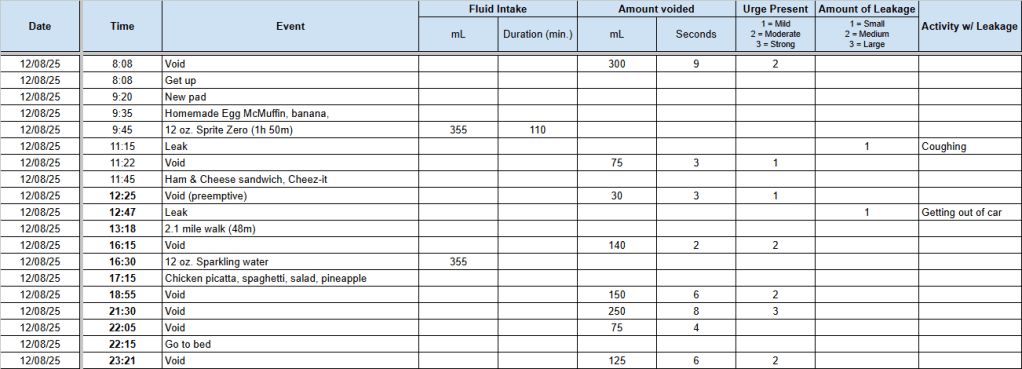
The cold started out with a light fever and lots and lots of coughing. Of course, when you have your prostate plucked from your pelvis and they zap what’s left, stress incontinence is an issue. If I have a light cough, I’m generally okay, but with this virus, I was having deep coughs where it seemed as though I was trying to turn my lungs inside out. I had to switch to the heavy-duty incontinence pads and, even then, I blew out two of them with coughing fits, leaking into my underwear and jeans. Messy and not fun.
The doctor gave me something to calm the dry coughs, and that had a bit of a positive effect. But then my sinuses filled, my nose was running, and I was coughing up phlegm so I switched to something else to deal with that.
Long story shorter, it’s pretty much all behind me now, and that’s a good thing. Maybe I’ll go back to the COVID days and wear masks when riding packed transit or wandering the halls of hospitals.
While I was down for the count, I had plenty of time to dig into more about androgen deprivation therapy (ADT), its pros and cons, and the timing of starting it. Sadly, I could find information that supported pretty much any perspective you wanted, which really isn’t all that helpful.
On the whole, it appears the current thinking is to start ADT sooner rather than later, and to use a doublet therapy, i.e., ADT + ARPI. This seems to delay time to metastasis, but has the obvious cost of substantial side effects.
On a related note, I called UCSD on 30 April to set up a second opinion appointment with the medical oncologist that’s well-respected and that the VA called to consult on my case two years ago. Because I was already in their system, that helped a little. I had to update my insurance information, and they said they’d get back to me in 2-3 business days. They didn’t, so I called back today, 11 May. They put me on the “high priority” call-back list this afternoon to be called back “between now and 48 hours.” Okie-dokie. And they say scheduling appointments at the VA is difficult…
I’ve got a number of appointments coming up at the end of May and into June:
27 May – PSA Test and other pre-ADT labs ordered by the oncologist
2 June – Meeting with VA medical oncologist
17 June – Dexa Scan bone density scan for baseline
23 June – Meeting with VA urologist
With luck, I’ll be able to add the UCSD medical oncologist to that list as well.
I really want the PSA test results—specifically, the PSA doubling time—to be a guide into what happens next and when.
One of the other things that I dug into a bit when I was down with the cold was how many values to use when calculating PSADT. As expected, there were dozens of different answers. Grr. My pea-sized engineer’s brain decided that I’ll use the last four PSA values if they cover at least a year. To me, that would render more useful information that shows the latest trend versus loading in all data points that may skew the results to show something less aggressive. But what do I know?
Using the Memorial Sloan-Kettering PSADT calculator and four data points over the last year, my PSADT is 8.9 months. Using a second calculator I found, it’s 8.21 months. For grins and giggles, I plugged in the last two years worth of data, and my PSADT was 10.4 months. Doing my research on ADT, PSADTs in the 6-9 month range seemed to be a trigger for action.
My PSA in March was 2.52 ng/mL, and I suspect it will be approaching 3.0 ng/mL at the end of May.
Obviously, this summer will be a series of data collection, evaluation, and big decision-making. Yippee! <sarcasm font>
Stay tuned for more.
Be well!
Header image: Torrey Pines State Beach, California