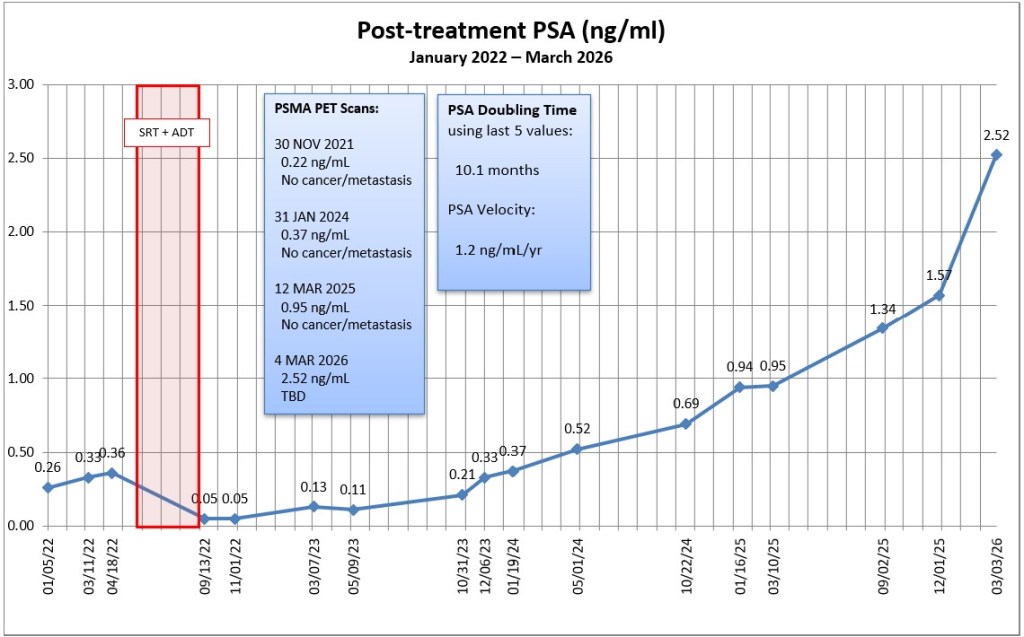
After last week’s PSMA PET scan, I did a little more digging into how the scans work, and why they don’t work for 10% to 20% of patients.
Prostate specific membrane antigen (PSMA) is a protein that’s found in healthy prostate cells, and it continues to exist in prostate cancer cells in most, but not all, cases.
PSMA in Imaging
Researchers found a way to attach a radioactive tracer to the PSMA proteins which would light up when seen in a PET scan, indicating the presence of cancer. Gallium-68 is the most commonly used tracer, with fluorine-18 also being used.
When the tracer is injected into the patient, it seeks out cells that have expressed the PSMA protein and attaches to them. The PET scanner then looks for areas where there is a build-up of the tracer to indicate where the cancer is located.
I’m going to use a grossly over-simplified analogy based on my reading as a lay person.
We all know that magnets are attracted to steel or iron. Imagine that the cancer cells with the PSMA protein are small steel ball bearings, and the radioactive tracer is a bunch of tiny magnets. Inject the magnets into your system, and they go in search of the steel ball bearings. When they find them, they attach, and the PET scan can see where all the magnets are located.
But for those patients whose cancer cells do not have the PSMA protein, that essentially means that the cancer cells are plastic balls, and the magnets that were injected will never attach to them. The PET scan won’t see any build-up of magnets/cancer cells.
Based on my experience with four PSMA PET scans, I believe that I’m in that 10% group and that my cancer cells do not express the PSMA protein—they’re the plastic balls.
PSMA in Treatment
In addition to using PSMA positive cells for imaging purposes, researchers have also recently developed a treatment that uses the PSMA positive cells. It goes by the brand name Pluvicto, but also known as Lutetium-177–PSMA-617.
It’s only used on patients with castration-resistant prostate cancer that have PSMA proteins.
The difference between using gallium-68 or fluorine-18 and lutetium-177 is that the lutetium is a radioactive material that attaches to the PSMA protein cells and delivers beta particle radiation to kill the cells.
This means that for those patients whose cancer doesn’t express the PSMA protein, this treatment option would not be available.
Alternative Imaging
On the good news front, there are other imaging options out there, one of which is Axumin (18F-fluciclovine). Instead of targeting PSMA in the cancer cells, it looks at the amino acids.
Axumin scans aren’t as sensitive as PSMA PET scans, but they are more sensitive than choline-11 scans.
At my current PSA level (2.52 ng/mL), the Axumin scan should have a decent chance of finding something.
In a conversation in a prostate cancer forum, I learned that one patient had used the gallium-68 tracer for his PSMA PET scans with the same results as mine, but they switched to PYLARIFY (piflufolastat F 18) as the tracer (which also attaches to the PSMA) and found four lesions using the different radiotracer. I know that one anecdotal case doesn’t mean much, but it’s something I can ask my team about.
Skip Imaging?
You may recall that, at one point, I had conflicting guidance from the urologist and oncologist on when to start androgen deprivation (hormone) therapy (ADT). One said when we saw metastasis, and the other said when my PSA hit 2.0 ng/mL. Clearly, I’ve passed the 2.0 threshold with my latest PSA results.
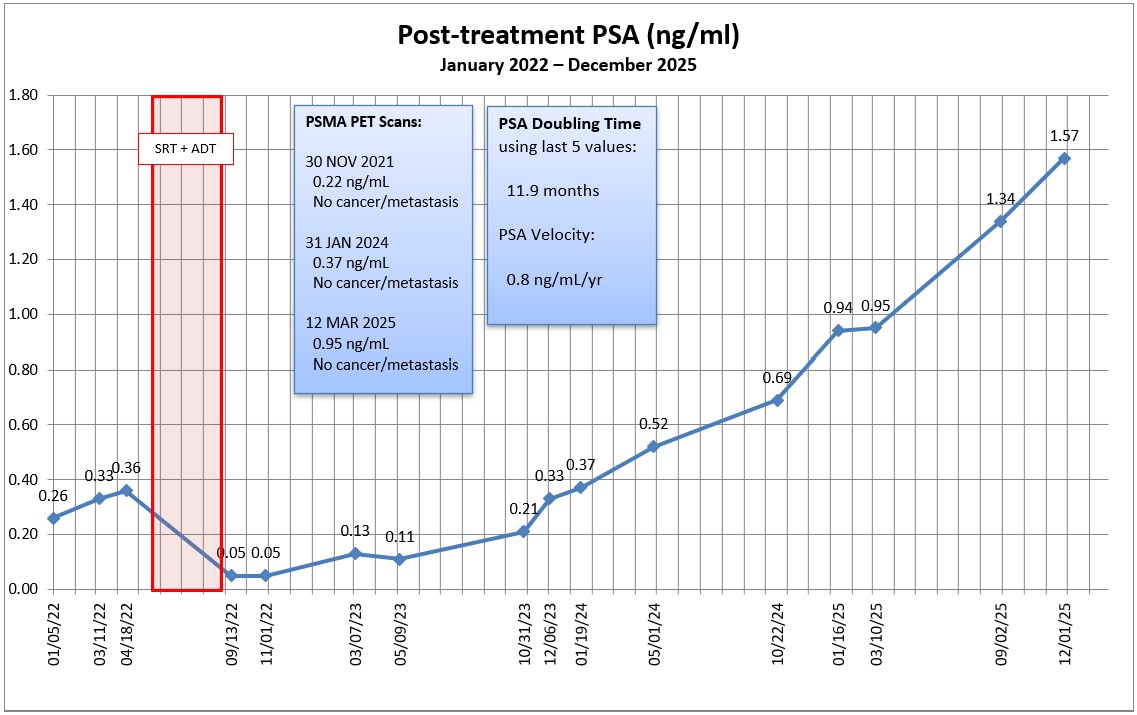
I went back and recalculated my PSA doubling time using only the last four values dating back to 10 March 2025. (The fourth and fifth values that I used before are 0.94 (January 2025) and 0.95 (March 2025), so having them so close may have skewed the results a little. When I used all five data points, my PSADT was 10.1 months; when I use the last four data points, it’s 8.9 months.
Given I’m past the PSA threshold (for one doctor) and the fact my PSADT is less than 10 months, I’m also wondering if there’s any value in continuing in the efforts to try and find the lesions. Or is is better, given how my PSA is increasing, to go ahead and just resign myself to the fact that I have micrometastases someplace and start the ADT sooner rather than later? In the time that it takes to schedule another scan, regardless of the type, my PSA could be well over 3.0 and even pushing 4.0.
That leads me to another question. If we do start the ADT and it knocks my PSA down to <0.1 like it did when I had it for salvage radiation therapy, does that mean that scans wouldn’t be able to locate the cancer while on ADT?
To my way of thinking, knowing where the cancer is at is important, even if it means letting the PSA run unabated for a short while longer. But what the hell do I know? I’m all ears for experiences from others that may have been in the same or similar situation.
Summary
Again, this is my lay person interpretation of things that I’ve researched, so please take this with a pound of salt. If you know I’m wrong on my interpretation, please let me know and provide references as to why I’m wrong. I want to learn.
You can rest assured, though, that this will be a part of my conversation with my team on 24 March.
Stay tuned for more.
Be well.
Header image: Desert wildflowers, Anza-Borrego Desert State Park, California