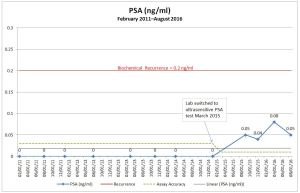
I really don’t have much to share in the way of prostate cancer-specific information, especially after last week’s post, Life After Radical Prostatectomy: 72 Months Later, so here are some random thoughts on living life.
Since that post last week, I managed to celebrate the 30th anniversary of my 29th birthday with some long-time, close friends. Woo-hoo! Any birthday you’re around to celebrate is a great birthday, no matter how many fire trucks show up to extinguish the candles on your cake. (Although I’m really not sure how easily I’ll embrace next year’s “milestone” birthday. Ugh!)
For some inexplicable reason, I seem to be more energized at the beginning of this new year compared to new years in the past. And, interestingly, that energy seems to be zeroing in on my creative side, with my photography being the intended focal point for that energy. (Pun not intended. Honestly.) I’ve discovered a couple of contemporary photographers on YouTube who have inspired me to hone my skills. I hope I can keep the momentum going.
I also want to work more on the social side of my life, but that’s going to be far more complicated than calculating the correct exposure settings on my camera. Okay. Perhaps complicated isn’t the right word. Being the introvert that I am, it will be challenging to get me out of my comfort zone. (Yes, the guy who talks openly about bodily functions is an introvert.)
Lastly, I just wanted to take a moment to talk about you at the beginning of this new year.
When I started this blog six years ago to keep family and friends informed (I refused to join Facebook back then), I had no idea that I’d still be here blogging six years later, and that my audience would grow to over 250 people from New Zealand to Canada to the United Kingdom and places beyond. Amazing. And quite humbling, too. So thank you for your continued support, interest, and friendship over the years. For 2017, I’ll recommit to providing meaningful, relevant content that’s of value to anyone else going down this path. (And if my writing isn’t that compelling, perhaps an awesome photo or two will hold your interest.)
All the best in 2017!
P.S. Oops! As I was prepping this post for publication, I noticed that I never did publish my Month 73 post last month. Too busy living life, I guess. That, or perhaps it has something to do with the 30th anniversary of my 29th birthday.