Those of us of a certain age may remember the “Stump the Band” segment on the Johnny Carson show, where audience members asked the band to play some obscure song. Well, today was my turn at “Stump the Urologist.”
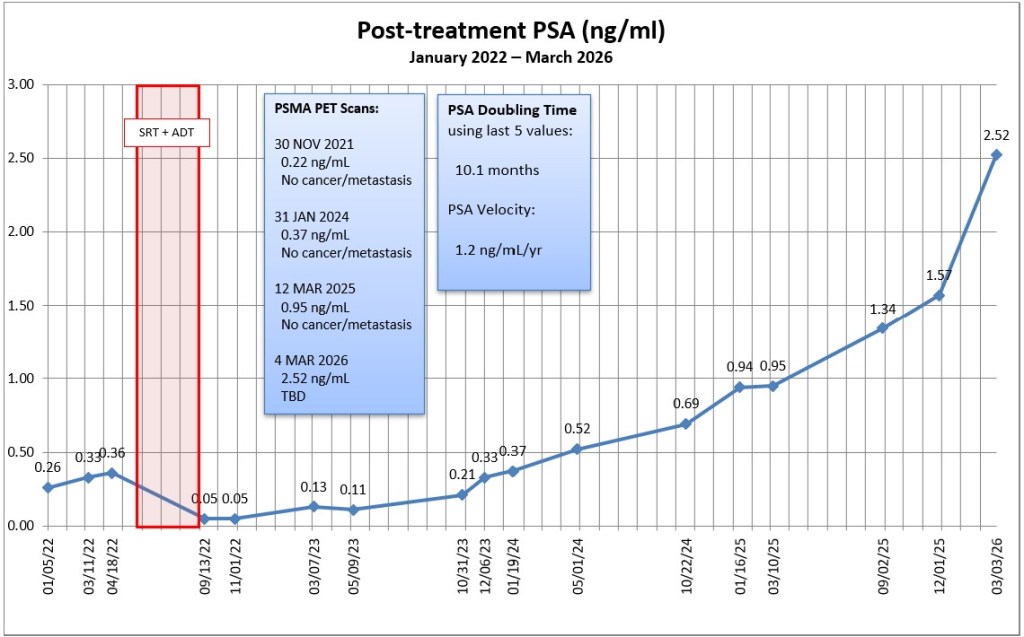
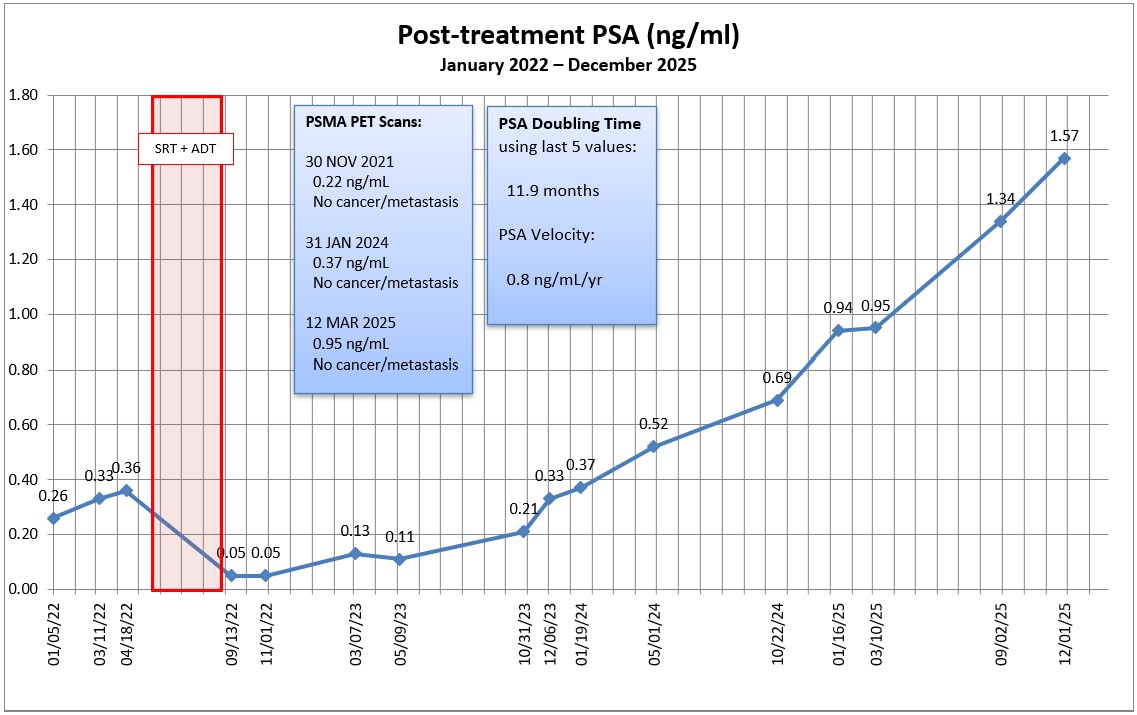
It was a very productive meeting that lasted nearly 40 minutes which was unusual. I came equipped with hard copies of my PSA chart, the MSKCC PSA doubling time (PSA-DT) calculator results, and my list of questions. He was impressed and really pleased with the chart in particular.
We started talking about how my four PSMA PET scans were all inconclusive, and I steered the conversation to whether I might be one of the 10% for whom PSMA PET scans don’t work. He seemed to be a bit skeptical at first, but he also said it was a possibility.
Given that my PSA increased substantially and my PSA-DT was decreasing, I wondered if it would be better to jump into ADT sooner or if there’s still value in trying to find the cancer’s location with imaging. He was of the opinion to continue to try to find it before starting ADT.
I had a series of questions that really dealt specifically with ADT, and he said it was a bit premature to think about those and that they would be better answered by a medical oncologist. I knew that I was jumping the gun with some of them, but I thought I’d ask anyway. During that part of the conversation, I did mention that I tolerated the ADT probably better than most when I had it for my salvage radiation therapy, but that I wasn’t eager to jump into it earlier than necessary.
After that, he took control of the conversation and asked me about my status when it came to sexual function and incontinence, and offered up options to deal with both if I was interested.
Then we returned to the topic of next steps, and that’s where I played “Stump the Urologist.” (Who, by the way, was a full-blown internist and not a resident.) He grabbed my PSA chart and excused himself for a few minutes as he went off to consult with the department head.
When he returned, I was a bit surprised when he put his faith in the results of the PSMA PET scan, saying it has the best sensitivity and the best specificity of any scan out there. He said that they had moved away from the Axumin scans because they were the old technology.
I politely pushed back, reminding him that a PSMA PET scan should have had an 80% – 90% chance of finding my cancer at my PSA level if I had the PSMA protein for the 68-Gallium tracer to lock onto. But if I don’t have that PSMA protein, the sensitivity and specificity of the scan won’t matter because nothing will ever light up. He really couldn’t argue against that.
I went back to the topic of ADT and mentioned that I met with a medical oncologist (MO) two years ago, and received conflicting opinions on when to start ADT. The MO said she would start my ADT when my PSA hit 2.0 ng/mL (a urologist said she wouldn’t start it until there was evidence of metastasis). Today’s urologist said he looks for one of three “triggers” to begin ADT: PSA > 10.0 ng/mL 😲; PSA-DT less than six months; or evidence of metastasis.
I also mentioned that the VA MO that I saw two years ago was a general oncologist and not someone who specialized in genitourinary cancers and, as helpful as she was, she had to consult with a UCSD MO who specifically deals with prostate cancer. I sowed the seed of eliminating the VA MO as a middleman if they have to consistently consult the UCSD doctor (who is highly regarded in the field), and suggested that I could just see him directly. I’m not sure if that will take root.
Finally, I did ask a very basic question given how elusive this has been: Is this even cancer? He said that, if I hadn’t had a prostatectomy, that there might be other explanations for the rising PSA. But he was confident that we are, in fact, dealing with cancer.
That led to a follow-up question of: Is it metastatic? Based on the information we have, he said it’s not. He seemed to squirm a bit when I asked about it being micro-metastatic, because, in his mind, that wasn’t very well-defined.
Before mapping out a plan, I have to admit that my ego puffed up a tad when he said, “You’re the best educated patient I’ve seen in weeks.” He also admitted that my case was a bit puzzling to them and not something they routinely see.
We agreed on three actions:
- The doctor is going to explore how and where I can get an Axumin scan, and if the VA will authorize it if I have to go outside the VA. That may take a day or two to get an answer. I mentioned that I’d be willing to use Medicare and go out on my own if necessary.
- He is doing a referral to get me seen by the VA oncology team to get them familiar with my case. I suspect it will take a few days to hear from the scheduler.
- We do another PSA test in June and meet to see where we’re at.
All in all, this was a good meeting with a robust discussion about my case that has all of us scratching our heads as to what’s going on and what to do next. Frustrating? Yes, to a degree. But, as we discussed during the meeting, nothing is black-and-white in the world of prostate cancer.
More to come.
Be well!
For my readers outside the U.S. who may not be familiar with Johnny Carson, I was going to link a random video clip of his “Stump the Band” segment above and, when I searched YouTube, this—of all clips—was the one that popped up first. I think you’ll see the related humor in it once you watch it. 😂
Header image: Anza-Borrego Desert State Park, California